Making Sense of Innovations in Primary Care
Here are the highlights from my talk on December 10, 2021 at the VCU Da Vinci Center for Innovation.
What is primary care?
Primary care means different things to different people. Patients experience it, clinicians deliver it, academics pontificate about it, and entrepreneurs redefine it. Traditionally, primary care is thought of as encompassing 4+ C’s including:
First Contact — seeing undifferentiated patients,
Comprehensive — providing acute, chronic and wellness care,
Continuity — following patients over their lifetimes,
Care Coordination — helping patients navigate the fragmented healthcare system.
These principles are foundational to achieving the Quintuple aim from the perspective of managing the health of populations. This aim started out Triple Aim to provide better patient care, better health outcomes, and lower cost, then Quadruple Aim included better workforce experience, and Quintuple aim now adds health equity as a priority.
In 2018, half of the ambulatory care visits were to primary care physicians.
Who delivers primary care?
The specialties
No consensus here either. Traditionally, it’s family medicine, pediatrics, and internal medicine. Some researchers include Obstetrics and Gynecology and Psychiatry. More realistically, it’s Urgent Care and Emergency Medicine for many patients that do not have a true primary care physician.
For a deep dive, see The State of Primary Care in the United States: A Chartbook of Facts and Statistics.
The “providers”
About ⅓ of physicians are in primary care and only ¼ of graduating medical students are entering primary care. The AAMC predicts primary care physician shortage to be between 18–48K in 2034.
Nurse practitioners can practice independent of physician supervision in 25+ states.
Physician Assistants rebranded themselves as Physician Associates in May of 2021.
Pharmacists have expanded their scope of practice. For example, in Florida they are able to start, change, and discontinue medications for many common conditions such as diabetes, asthma, COPD.
Entrepreneurs armed with AI are shaking up the primary care landscape. Money flowing into digital health is at all-time record-breaking numbers with $20+ billion in 2021.

I can’t help but juxtapose the 1948 LIFE magazine photo essay of Dr. Ceriani, the country doctor who makes house calls, delivers babies, and performs surgery on the elderly alongside AI chatbots like Buoy Health that empower patients to make sense of their symptoms and find definitive care from their connected devices.
Primary care is changing
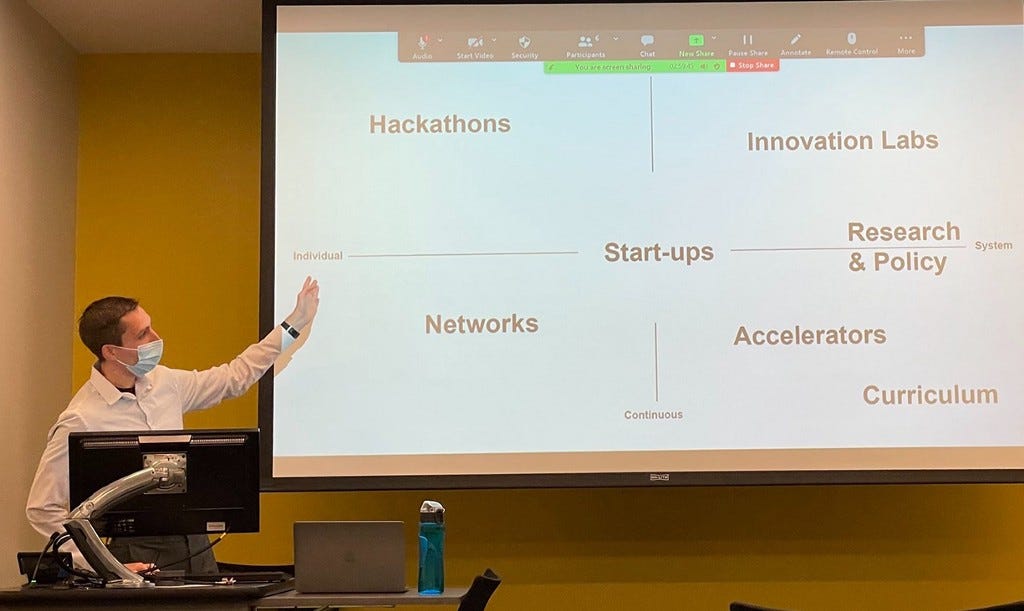
But not all change is innovative. I think of innovation as change that adds value to what already exists. Some changes in primary care are simply alternatives to the poorly functioning status quo and offer variable levels of added benefit. With so much happening at a rapid pace, we need a framework to contextualize the mechanisms of innovation (MOI) in primary care. To keep things simple, we’ll dive into seven MOIs charted on two dimensions in Figure 1: level of impact (horizontal axis) and time horizon (vertical axis).

Hackathons
Hackathons are 24 to 48 hours sprints of experimentation, collaboration, and prototyping with kindred creative change makers. They are not just for computer programmers, although that’s how it all started in 1999 as a challenge to write code for a handheld device. It wasn’t until 2010 when the first healthcare hackathon took place at Health Datapalooza to build upon then newly created HealthData.gov.
Examples of recent hackathons and their themes in 2021:
Rutgers Biomedical Entrepreneurship Network (BEN) — Health Equity;
VCU HealthHacks — Reimagining Medical Education;
Jefferson Health Hack — From COVID Madness to Mental Health.
Do they work? Some argue they are dangerous, while others point to data that show they are effective in generating value in the real world. Success stories abound as well, such as creation of PillPack in 2012 at MIT Hacking Medicine hackathon, and was eventually acquired by Amazon in 2018 for more than $750 million.
Networks
I define networks as online communities that facilitate connections through webinars, Zoom fireside chats, virtual coffee meet-ups. I am going to highlight a few Slack-based groups that are fairly active. Some are fee-based, others are open-invite. None are focused exclusively on primary care, but include primary care related content.
DiMe (Digital Medicine Society) — non-profit, >1950 members;
MD++ connects medical students with start-up and venture capital opportunities;
NODE Health (Network for Digital Evidence in Health) — non-profit, includes 32+ healthcare systems, >750 members;
SoPE (Society of Physician Entrepreneurs) — paid membership, >450 members;
PI (Physician Innovator) — Canadian-based, >45 members.
Other networks to explore:
FMEC (Family Medicine Education Consortium) Innovators Network — presentations from recent meeting in October, 2021 available on FMEC YT channel with topics like “Community Owned Health Plan” and “Role of Primary Care in Affordable Housing”;
AMA (American Medical Association) Physician Innovation Network — includes active forums;
RedCrow — platform to preview early stage healthcare companies.
Start-ups
This is a huge segment and I’ll keep things at bird’s eye level. This is how investors and venture capital firms view markets in primary care, mobile health, wearables, and remote patient monitoring.



Unique delivery model
Direct primary care (DPC) is a subscription-based membership model for patients to contract directly with their physicians. Removing insurance companies from the doctor-patient relationship has enabled primary care physicians to provide high-touch patient care at affordable prices. More importantly, it’s a type of model that allows physicians to easily create their own start-up practices, which share the core model but are each unique in their own way. It’s rare for two DPC practices to be completely alike.
To learn more, dig into the following resources:
Facilitators
Incubators facilitate the growth of business ideas and accelerators facilitate the growth of entities that carry out those ideas. They overlap in mentorship and provide know-how for turning ideas into products and services. Few notable examples:
Digital.health has an extensive list of healthcare accelerators across the globe 🌎.
Brown Hatch Health at Brown University is an incubator focused on supporting ventures created by students.
High Value Health Care Incubator at Stanford Clinical Excellence Research Center offers support to non-profit clinics that care for underserved patients.
StartEx — sponsored by Ontario Medical Students Association Innovation Grant pairs up Canadian medical students and start-ups for immersive entrepreneurship experiences.
Innovation Labs
Innovation labs do not always have clear-cut goals and their true impact is difficult to measure. Some exist to signal innovation for their home institutions, while others are prolific in their creative output. Here are some of the more interesting entities:
Primary Care Innovation Lab at UW Family Medicine — emphasis on technology adoption in primary care via grants and contracts with health organizations and business partners.
HMS Center for Primary Care — supports wide-spanning primary care initiatives, including entrepreneurship and leadership development.
Center for Health Care Innovation at Penn Medicine has the Acceleration Lab (implementing and scaling new ideas); the Nudge Unit (behavioral design within a health system), the Center for Digital Health (non-traditional data leverage), and Way To Health (research-driven patient engagement platform).
UC Davis Cloud Innovation Center (CIC) is collaboration with Amazon Web Services (AWS) to create the first CIC at an academic medical center, and it’s focused on building digital health equity.
Research & Policy
True innovation drives policy. Research is the slow-burn of ideas that build policy to kindle innovation.
Robert Graham Center — supports the policy development and advocacy efforts of AAFP.
The Green Center — primary care research engine with research notable for person-centered primary care measures.
Institute for Healthcare Improvement — founded by Don Berwick in 1991 to drive quality improvement in health care and includes IHI Open School for training in improvement and safety.
Curriculum
Expanding educational opportunities for primary care trainees has the potential to create a new generation of thought leaders. Weighed down with historical inertia of doing things the way they have been done in the past, change in academia is sluggish. The bright side is that you can arrive several decades late to medical education and still be innovative.
Dell Medical School in partnership with Texas Health Catalyst offers a semester-long Associate Program with the goal of working on interdisciplinary teams to learn about healthcare technology commercialization and develop leadership skills. Its CoLab serves as the hub for product innovation, networking and entrepreneurship for trainees and their educators. Dell third year medical students have a 9-month “Innovation, Leadership, and Discovery” block.
Sidney Kimmel Medical College at Thomas Jefferson University has the first co-curricular design thinking program at a US medical school.
Medical Innovators Development Program at Vanderbilt School of Medicine — innovation-centered four-year curriculum for those with a science PhD who are also completing their medical training. While not primary care-oriented, there is potential for similar programs to be adapted for primary care trainees.
Charting the future terrain of primary care is an exciting experience that does not have to happen in isolation. After all, most innovation require collaboration and exchange of ideas. Lots of ideas. We have a lot to learn from each other, and I would love to hear your thoughts on what’s emerging in primary care.



